Last Updated: April 24, 2026 | v1.0
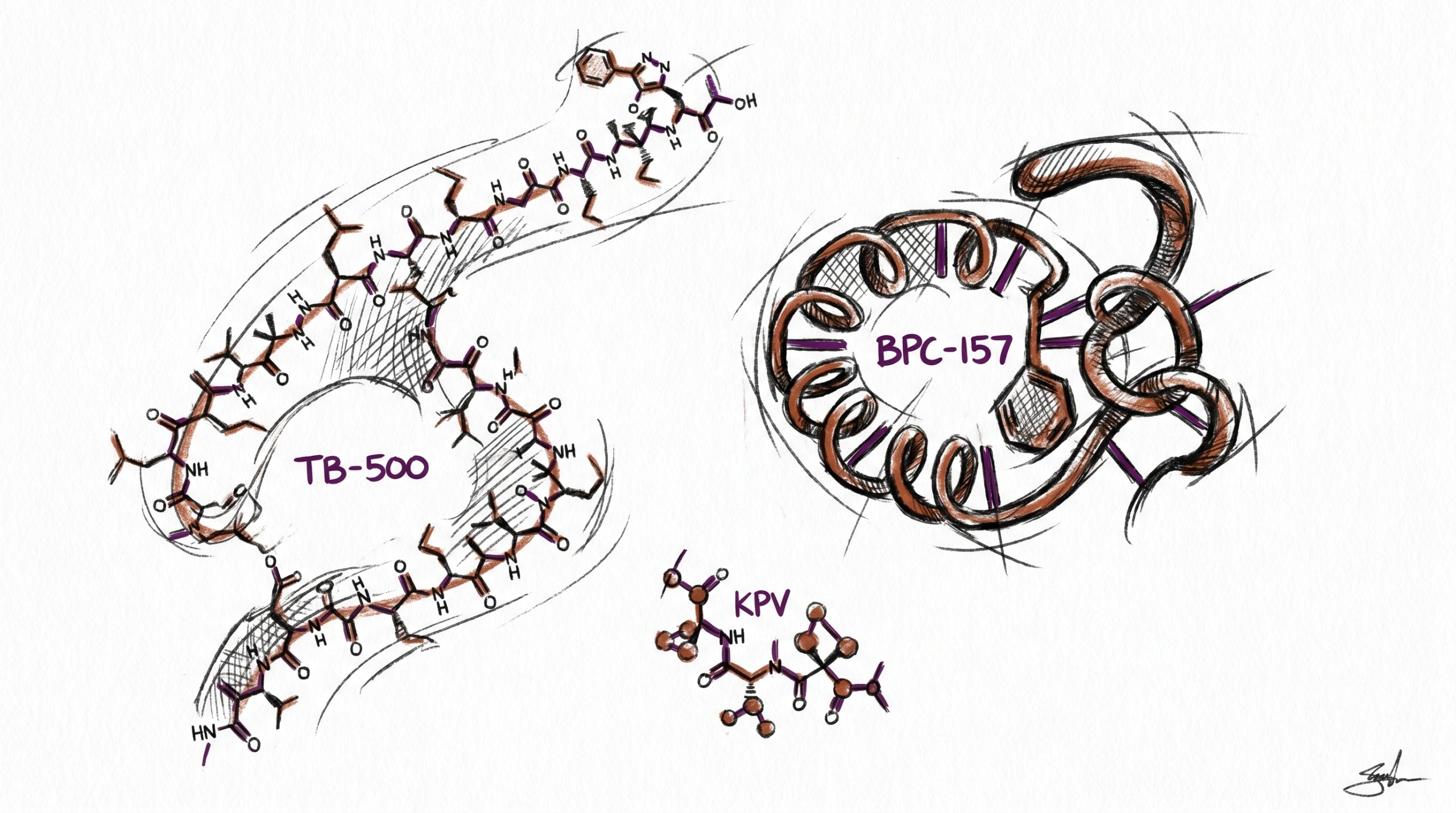
TB-500, BPC-157, and KPV are three research peptides widely studied for their roles in tissue repair, regenerative biology, and inflammation modulation in preclinical models. Each operates through a mechanistically distinct pathway: TB-500 is a 43-residue derivative of the actin-sequestering protein Thymosin Beta-4, BPC-157 is a 15-residue partial sequence derived from human gastric juice with cytoprotective properties, and KPV is a tripeptide α-MSH C-terminal fragment (residues 11-13) with anti-inflammatory activity. Although all three are frequently grouped under the “healing peptide” umbrella in research literature, their molecular architectures, receptor interactions, and downstream signaling cascades differ substantially. This guide compares the three side by side: mechanism, molecular characteristics, published preclinical research, and how investigators choose among them for specific tissue-repair protocols. All products and information are provided for laboratory and research purposes only.
Quick Comparison: TB-500 vs BPC-157 vs KPV
| Attribute | TB-500 | BPC-157 | KPV |
|---|---|---|---|
| Parent molecule | Thymosin Beta-4 (Tβ4) | Body Protection Compound from human gastric juice | α-Melanocyte-Stimulating Hormone (α-MSH) |
| Sequence length | 43 residues (full Tβ4) or LKKTETQ fragment (7 residues) | 15 residues | 3 residues (Lys-Pro-Val) |
| Molecular weight | ~4,963 Da (full Tβ4) | ~1,419 Da | ~343 Da |
| Primary mechanism | Actin sequestration; cell migration; angiogenesis | Modulation of nitric oxide, VEGFR2, and growth hormone pathways; cytoprotection | Melanocortin-independent anti-inflammatory signaling; NF-κB modulation |
| Primary research applications | Cardiac tissue repair, wound healing, corneal regeneration | Gastrointestinal repair, tendon and ligament models, vascular research | Colitis research, dermal inflammation, mucosal healing |
| Orally stable? | No (parenteral research use) | Published stability in preclinical oral protocols | Yes (tripeptide size) |
What Is a Healing Peptide in Research Contexts?
The term “healing peptide” is a functional, not chemical, classification used in research literature to describe short peptide molecules that modulate pathways involved in tissue repair, angiogenesis, inflammation resolution, and cellular migration. Unlike hormone mimetics such as GLP-1 agonists, healing peptides do not typically bind a single canonical receptor. Instead, each one engages a distinct constellation of intracellular targets, cytokine pathways, and signaling second messengers. TB-500 acts primarily through intracellular actin binding; BPC-157 appears to operate through a network of vascular and neurogenic signals that remain incompletely mapped in published studies; KPV exerts anti-inflammatory effects independent of melanocortin receptor binding. Grouping them together reflects the shared research interest in tissue repair, not a shared molecular class. Investigators designing regenerative-biology studies often screen candidates from each category separately before considering combination protocols.
From a molecular biology perspective, the three compounds also differ dramatically in size. TB-500 in its full Thymosin Beta-4 form is a 43-residue actin-binding protein of roughly 4,963 Daltons, while the synthetic fragment commonly studied under the TB-500 label is a shorter 7-residue sequence (LKKTETQ) corresponding to the active actin-binding domain. BPC-157 is a 15-residue sequence (GEPPPGKPADDAGLV) of approximately 1,419 Daltons, derived from a 40-kDa parent protein isolated from human gastric juice. KPV is the smallest of the three, a simple tripeptide (Lys-Pro-Val) of about 343 Daltons corresponding to the C-terminal end of α-melanocyte-stimulating hormone. This size spectrum has practical consequences for stability, route-of-administration research, and pharmacokinetic modeling in preclinical protocols.
How Does BPC-157 Work in Preclinical Research?
BPC-157, or Body Protection Compound-157, is a 15-amino-acid partial sequence derived from a larger protein originally isolated from human gastric juice. Its sequence (GEPPPGKPADDAGLV) has been characterized in published preclinical literature for over two decades, with the majority of the foundational work emerging from the Sikiric laboratory and collaborators. In preclinical models, BPC-157 appears to promote healing through a multi-pathway mechanism that includes upregulation of vascular endothelial growth factor receptor 2 (VEGFR2), modulation of the nitric oxide (NO) system, and interactions with the growth hormone and dopamine signaling pathways. Published studies suggest BPC-157 accelerates tissue repair in gastrointestinal, tendon, ligament, and vascular research models, with notable cytoprotective effects on mucosal integrity and endothelial function. Investigators studying these pathways can source BPC-157 from Peptideware with batch-specific HPLC verification.
A distinctive feature of BPC-157 in the published literature is its reported stability across multiple preclinical routes of administration, including oral, intraperitoneal, and subcutaneous, without reliance on a specific carrier or enhancer. Preclinical research indicates BPC-157 resists degradation in gastric acid and maintains biological activity after oral delivery in rodent models, a property that distinguishes it from most peptides of comparable size. Mechanistically, published reviews have emphasized BPC-157’s interaction with the NO pathway: it appears to counteract the effects of NO-synthase inhibition and to restore endothelial NO signaling after injury. The broader “body protection” hypothesis in the literature proposes that BPC-157’s parent protein acts as a homeostatic modulator in the gastric mucosa, and that the 15-residue fragment retains a core subset of those regulatory activities. This remains an active area of published investigation, and researchers designing mechanistic studies should consult the primary literature for each specific endpoint.
How Does TB-500 Differ as an Actin-Binding Peptide?
TB-500 is the research-grade designation for a synthetic peptide based on Thymosin Beta-4 (Tβ4), a 43-residue, 4,963-Dalton actin-sequestering protein found in nearly all mammalian cells. Tβ4 is the most abundant member of the beta-thymosin family and functions intracellularly by binding G-actin monomers in a one-to-one stoichiometric ratio, maintaining the pool of unpolymerized actin that cells draw on for dynamic cytoskeletal remodeling. Because cell migration, proliferation, and wound closure all require controlled actin polymerization, Tβ4 occupies a central role in preclinical tissue-repair research. The commercially circulated “TB-500” label refers interchangeably to either the full 43-residue recombinant Tβ4 or to the shorter 7-residue active fragment LKKTETQ, which corresponds to the actin-binding domain. Research-grade TB-500 is available through Peptideware for investigators studying actin-cytoskeleton dynamics.
Beyond direct actin sequestration, published studies have characterized additional roles for Tβ4 in angiogenesis, cardiac progenitor cell activation, and corneal epithelial regeneration. Preclinical research indicates Tβ4 upregulates VEGF expression and promotes endothelial cell migration, which contributes to the revascularization phase of wound healing in animal models. The TIME-1 and TIME-2 cardiac studies and subsequent preclinical cardiac repair literature have examined Tβ4’s ability to activate epicardium-derived progenitor cells after ischemic injury in rodent models. Corneal research has also used TB-500 in topical protocols to study epithelial healing after controlled abrasion. Because Tβ4 operates primarily through an intracellular target, its delivery and cellular-uptake properties are active research questions; published studies have used both recombinant full-length Tβ4 and synthetic fragments with broadly similar preclinical outcomes, though head-to-head comparisons of the two forms in identical models remain limited.
What Makes KPV Unique as an Anti-Inflammatory Fragment?
KPV is a simple tripeptide consisting of lysine, proline, and valine (Lys-Pro-Val), corresponding to residues 11-13 at the C-terminal end of α-melanocyte-stimulating hormone (α-MSH). Despite its extreme brevity, KPV retains a significant portion of α-MSH’s anti-inflammatory activity in preclinical research models. Unlike the parent α-MSH molecule, KPV does not bind the melanocortin receptors with meaningful affinity; instead, published studies indicate KPV operates through a melanocortin-independent mechanism involving direct intracellular effects on nuclear factor kappa-B (NF-κB) signaling and reduction of pro-inflammatory cytokine production including TNF-α and IL-6 in cellular models. Investigators studying mucosal and dermal inflammation can source KPV from Peptideware as a 10 mg lyophilized preparation.
The tripeptide’s small size carries significant practical advantages in research. At approximately 343 Daltons, KPV crosses epithelial barriers more readily than larger peptides and has been studied in oral, topical, and intracolonic preclinical protocols. Colitis research, in particular, has featured KPV because of its reported ability to reduce mucosal inflammation in rodent dextran-sulfate-sodium (DSS) colitis models. Published studies suggest the anti-inflammatory effect extends to cutaneous models, with topical KPV applications studied in dermatitis and wound-inflammation research. KPV is often grouped with BPC-157 in healing-peptide research because both operate without requiring classical receptor binding at a single target, though the downstream pathways differ substantially: BPC-157 engages vascular and NO signaling, while KPV acts more directly on cytokine transcription pathways. Researchers selecting among them should match the target inflammatory context to the documented mechanism.
How Do These Compounds Compare in Published Research?
The published literature on each of these three peptides has matured along distinct trajectories. BPC-157 has the deepest single-laboratory publication record, with decades of work from the Sikiric group and growing independent replication in preclinical gastrointestinal, musculoskeletal, and vascular models. TB-500 and the broader Thymosin Beta-4 literature have been shaped by cardiac and ophthalmic research programs and by industry-funded clinical investigations into wound healing. KPV’s literature is smaller but tightly focused on mucosal and cutaneous inflammation, with a notable cluster of colitis-model publications. Investigators evaluating these compounds for their own research should assess the quantity, independence, and methodological rigor of the published body of work for each target endpoint.
| Compound | Primary research area | Representative model systems | Published literature characteristics |
|---|---|---|---|
| BPC-157 | GI mucosa, tendon, ligament, vascular | Rat colitis, Achilles tendon transection, gastric lesion | Large single-lab corpus, growing independent replication |
| TB-500 / Tβ4 | Cardiac, corneal, dermal wound | Murine myocardial infarction, corneal abrasion | Multi-laboratory, industry-sponsored preclinical and early clinical |
| KPV | Mucosal and cutaneous inflammation | DSS colitis, dermatitis, IBD-model | Smaller but focused; mucosal emphasis |
A critical consideration when comparing published data is the degree to which each compound’s mechanism is currently mapped. BPC-157’s breadth of reported effects exceeds what its incomplete mechanistic characterization can fully explain; researchers should treat reported outcomes as pathway-associated rather than as direct receptor-level findings. TB-500’s intracellular actin-binding mechanism is the most molecularly well-defined of the three, though its tissue-level pharmacology involves downstream angiogenic and migratory cascades that are themselves complex. KPV’s NF-κB-associated mechanism is supported by a smaller but consistent cellular-model literature. Investigators interested in the broader Healing Peptides category can review the Peptideware pillar guide for cross-compound context.
Which Healing Peptide Should Researchers Choose?
Choosing among TB-500, BPC-157, and KPV depends on the research question and the target tissue. For investigators focused on gastrointestinal mucosal repair, vascular integrity, or tendon and ligament models, BPC-157 has the largest published evidence base and is the logical first candidate. Its multi-route stability also makes it operationally flexible for preclinical protocols that require oral or intragastric delivery. For cardiac tissue repair, corneal epithelial regeneration, or studies centered on actin cytoskeleton dynamics, TB-500 is the more appropriate choice because its mechanism is tightly coupled to cellular migration and cytoskeletal remodeling. Its large molecular weight, however, typically limits research protocols to parenteral administration.
For investigators studying mucosal or cutaneous inflammation, particularly in colitis and dermatitis models, KPV offers a distinct mechanistic angle through NF-κB modulation and melanocortin-independent anti-inflammatory activity. KPV is also the only one of the three that is practical for high-throughput oral-route screening in rodent models because of its tripeptide size. Some published investigators combine BPC-157 and KPV in integrated protocols to probe both regenerative and anti-inflammatory arms of tissue repair, though interaction data in matched preclinical models remains limited. In combination-candidate research, the KLOW Blend, a four-peptide formulation of BPC-157, TB-500, GHK-Cu, and KPV, is circulated as a research-only preparation for multi-pathway exploratory protocols.
How Are These Peptides Reconstituted and Stored?
All three peptides are supplied as lyophilized powders in sealed vials and should be stored at -20 degrees Celsius for long-term stability. For research use, reconstitution with pharmaceutical-grade bacteriostatic water containing 0.9% benzyl alcohol is the standard protocol; the benzyl alcohol preservative enables multi-use vials across a typical 28-day reconstituted window. After reconstitution, all three should be stored at 2-8 degrees Celsius and protected from light. Reconstituted peptides should not be frozen, because ice crystal formation damages peptide bonds and degrades molecular integrity. Researchers should label each reconstituted vial with the date of reconstitution, concentration, and bacteriostatic water volume, and gently swirl rather than shake during reconstitution to preserve structural fidelity. Peptideware supplies bacteriostatic water in both 3 mL single-vial and 10 mL multi-use formats for preclinical protocols.
Frequently Asked Questions
Is TB-500 the same molecule as Thymosin Beta-4?
TB-500 is a research-market designation that is used interchangeably for either full-length Thymosin Beta-4 (a 43-residue, 4,963-Dalton protein) or for a shorter synthetic 7-residue fragment (LKKTETQ) that corresponds to the active actin-binding domain. Preclinical research has used both forms, with broadly similar tissue-repair outcomes in published models, though direct head-to-head comparisons in matched protocols remain limited. Investigators designing mechanistic studies should confirm with their supplier which form the preparation represents and should consult the primary literature for each endpoint to determine which form was used in the reference study. Peptideware’s TB-500 is supplied as a lyophilized preparation with batch-specific HPLC verification and certificate-of-analysis documentation.
What is the functional difference between BPC-157 and KPV?
BPC-157 and KPV are both short research peptides associated with tissue repair, but they differ fundamentally in mechanism and target pathway. BPC-157 operates through a multi-pathway network that includes vascular endothelial growth factor receptor 2 (VEGFR2) upregulation, nitric oxide system modulation, and interactions with growth hormone and dopamine signaling. Its reported effects span gastrointestinal, musculoskeletal, and vascular research models. KPV operates through a more narrowly defined anti-inflammatory pathway, acting intracellularly on nuclear factor kappa-B (NF-κB) signaling and reducing pro-inflammatory cytokine transcription. Its primary research applications are mucosal (colitis models) and cutaneous (dermatitis models) inflammation. Researchers selecting between them should match the compound’s documented mechanism to the target inflammatory or regenerative context under investigation.
Can BPC-157, TB-500, and KPV be combined in research protocols?
Combination research using two or more of these compounds is an active but less-mature area of the published literature. The four-peptide KLOW research blend (BPC-157, TB-500, GHK-Cu, KPV) is one commercially circulated example of a combination preparation, and individual investigators have studied pairwise combinations in preclinical wound-healing and tendon-repair models. Published data are insufficient to characterize clear synergistic or additive profiles across model systems, and researchers interested in combination protocols should consult the primary literature for their specific endpoint and consider parallel-arm designs that compare individual compounds against the combination. Because the mechanisms are distinct, multi-pathway protocols are mechanistically plausible, but interaction data remain limited and should be interpreted cautiously.
Is KPV stable when administered orally in research?
KPV’s tripeptide size confers significantly better oral stability than larger peptides because the short sequence resists many of the proteolytic degradation pathways that rapidly cleave longer chains. Published studies have used oral, intracolonic, topical, and intraperitoneal administration routes in rodent colitis and dermatitis models, with biological activity demonstrated across delivery routes. This operational flexibility is one of KPV’s distinguishing characteristics in research literature. However, oral bioavailability is not 100%, and pharmacokinetic parameters vary across reported model systems. Investigators designing oral-route protocols should consult the primary literature for their target endpoint and should establish dosing ranges based on published preclinical data for the specific model in use.
How should these peptides be stored for research use?
All three peptides should be stored at -20 degrees Celsius in their sealed lyophilized vials, protected from light, where they remain stable for 12-24 months depending on preparation. After reconstitution with pharmaceutical-grade bacteriostatic water containing 0.9% benzyl alcohol, solutions should be transferred to 2-8 degrees Celsius refrigeration and used within 28 days. Reconstituted peptides must not be frozen, as ice crystal formation fractures peptide bonds and destroys molecular integrity. Vials should always be protected from direct sunlight and UV exposure, which accelerate oxidative degradation. Researchers should label each reconstituted vial with the date of reconstitution, concentration, and bacteriostatic water volume. Gentle swirling rather than vigorous shaking preserves structural fidelity during reconstitution.
What purity and verification should researchers require?
Research-grade BPC-157, TB-500, and KPV should be sourced from suppliers who provide third-party certificate of analysis documentation verifying peptide identity, purity (typically greater than 98% by HPLC), and absence of endotoxin contamination. Mass spectrometry confirmation of molecular weight provides additional identity verification and is especially important for KPV given its extreme brevity and sensitivity to sequence errors. Peptideware supplies all three peptides with batch-specific HPLC data and third-party mass spectrometry verification. For detailed evaluation criteria, researchers can consult the Peptideware Peptide Quality: Third-Party Testing guide, which describes purity standards and COA interpretation for preclinical procurement.
Are these peptides approved for human use?
No. TB-500, BPC-157, and KPV are supplied exclusively for laboratory and research purposes in preclinical model systems. None of the three compounds are approved by the FDA for human therapeutic use, and none should be used in any context outside controlled research environments. Peptideware’s products are sold with explicit research-use-only documentation, and researchers should ensure that all preclinical protocols comply with applicable institutional and regulatory requirements. The published literature referenced throughout this guide describes preclinical findings in animal and cellular models; translation to human therapeutic applications would require separate clinical investigation under regulatory oversight that has not yet occurred for any of these three compounds.
Summary
TB-500, BPC-157, and KPV are three mechanistically distinct research peptides studied for their roles in tissue repair, regenerative biology, and inflammation modulation in preclinical models. TB-500 operates through actin-binding and downstream angiogenic cascades, with primary research applications in cardiac, corneal, and dermal wound models. BPC-157 operates through multi-pathway modulation of vascular, nitric oxide, and growth-regulatory signaling, with the broadest published literature centered on gastrointestinal, tendon, and ligament research. KPV operates through melanocortin-independent NF-κB modulation, with research applications concentrated in mucosal and cutaneous inflammation models. Researchers selecting among them should match the compound’s documented mechanism and published evidence base to the specific research context, and should consult primary literature for pharmacokinetic and pharmacodynamic parameters before protocol design.
Research Disclaimer: All products are intended for laboratory and research purposes only. Not for human or animal consumption. These statements have not been evaluated by the FDA.